|
9/1/2023 0 Comments Plexiform layers 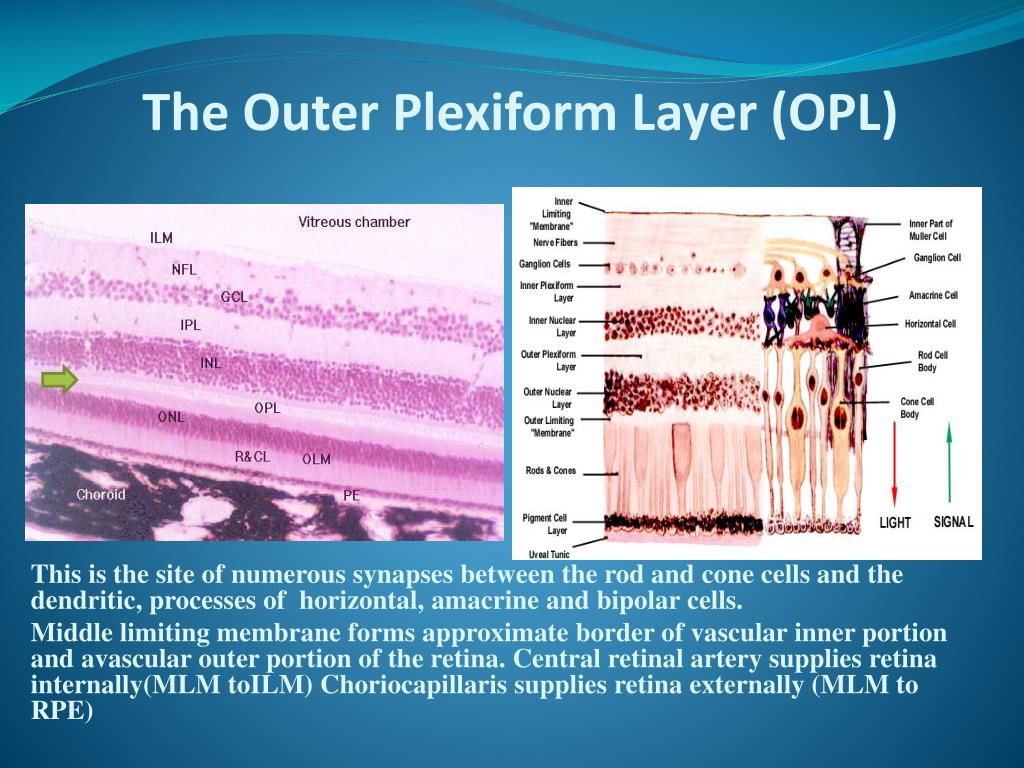
However, whether alterations in the intraretinal structure in patients with PD can act as an indicator for early diagnosis of PD remains unclear. Many previous studies have explored the alterations in retinal morphology of patients with PD in vivo using OCT imaging 9, 10, 11, 12, 13. High-definition optical coherence tomography (HD-OCT), a noninvasive optical imaging technique that allows cross-sectional retinal microstructure imaging quantitatively, has become an appealing candidate imaging modality in PD. The diagnosis of PD at an early stage remains challenging. These observations suggest that retinal pathological changes probably occur in patients with PD. 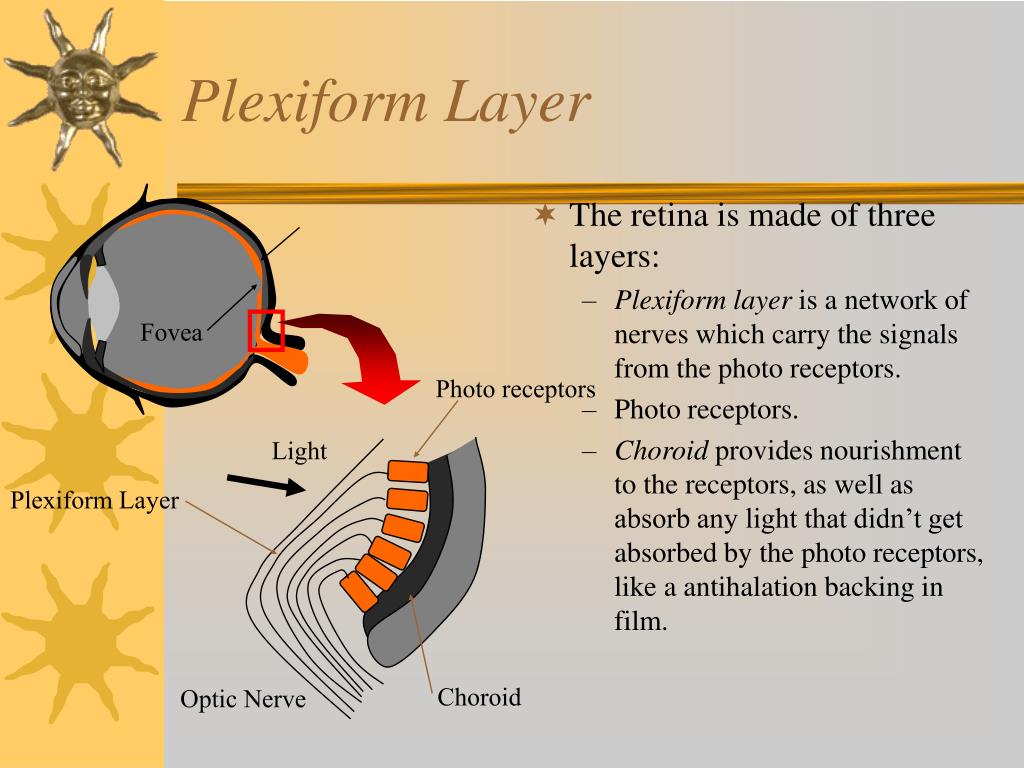
In addition, there are phosphorylated α-synuclein and Lewy body deposits in the retina of patients with PD 8. Studies have shown that the immunoreactivity of tyrosine hydroxylase in dopaminergic cells 5 and the retinal dopamine content in PD are decreased 6, 7. Their dendritic branch extends from the retinal inner nuclear layer (INL) to the inner plexiform layer (IPL), where it is connected to bipolar cells and retinal ganglion cells 4. Dopamine-containing amacrine cells play a role in integrating visual information. The retina, an extension of the central nervous system, has attracted significant attention in the brain pathological processes of neurodegenerative disorders in recent years 3. Apart from predominant motor symptoms, visual disturbances, such as impaired visual acuity, visuospatial dysfunction, and visual hallucinations, can also be observed in patients with PD 2. Parkinson’s disease (PD), characterized by selective loss of nigral dopaminergic neurons, is the second most common neurodegenerative disorder 1. Furthermore, macular IPL-SI thickness might be performed as an early diagnostic indicator for PD. In conclusion, we confirmed the retinal structure was significantly altered in patients with PD in different clinical stages, and that GCL and IPL changes occurred during early PD disease and were correlated with MDS-UPDRS III scores and non-motor symptoms assessment scores. Furthermore, macular IPL thickness in the superior inner (SI) quadrant (IPL-SI) had the best diagnostic performance in patients with PD with H-Y I versus HCs, with a sensitivity and specificity of 75.06% and 81.67%, respectively. In addition, we observed that GCL and IPL thicknesses were both correlated with Movement Disorder Society-Unified Parkinson’s Disease Rating Scale III (MDS-UPDRS III) scores and non-motor symptoms assessment scores. Moreover, the ganglion cell layer (GCL), inner plexiform layer (IPL), and outer nuclear layer were thinner in patients with PD with H-Y I, and significantly decreased as the H-Y stage increased. As a result, the PD group had a significantly lower average, temporal quadrant pRNFL, MRT, and TMV than the HCs group (all p < 0.001). The peripapillary retinal nerve fiber layer (pRNFL), total macular retinal thickness (MRT), and macular volume (TMV) were measured by high-definition optical coherence tomography, and the macular intraretinal thickness was analyzed by the Iowa Reference Algorithms. In total, 397 patients with PD and 427 healthy controls (HCs) were enrolled. We assessed the retinal layer thickness in different stages of PD and explored whether it can be an early diagnostic indicator for PD. Whether structural alterations of intraretinal layers are indicators for the early diagnosis of Parkinson’s disease (PD) remains unclear. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
